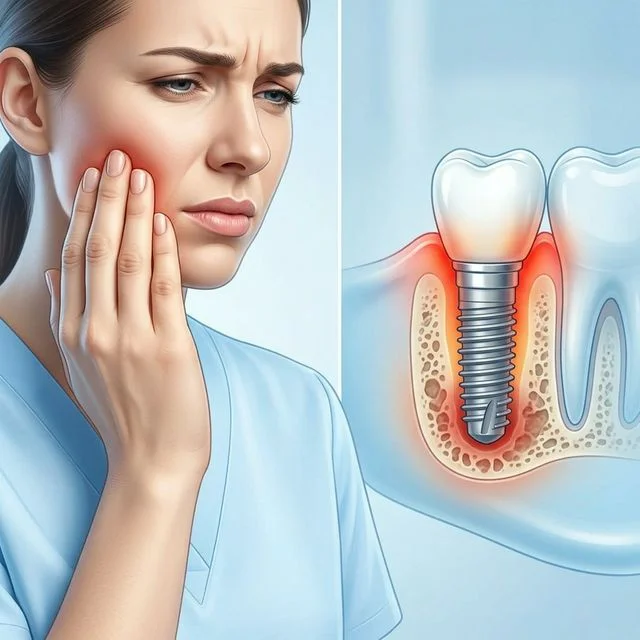
Dental implant surgery is one of the most successful procedures in dentistry, with a 95–98% success rate. But that doesn't mean it's painless. Whether you just had the procedure or you're dealing with pain months later, you need real solutions — not vague advice to "take it easy."
I'll walk you through exactly what to take, when to take it, what to apply, what to eat, and — critically — when your pain means something is wrong and you need to call your dentist immediately.
Pain Timeline: What to Expect
Understanding the normal pain timeline helps you know whether what you're experiencing is expected or concerning:
| Timeframe | What to Expect | Pain Level (1–10) |
|---|---|---|
| Day of surgery | Numbness wears off 2–4 hours post-op; dull ache begins | 2–4 |
| Days 1–3 | Peak pain & swelling; this is the worst it gets | 4–7 |
| Days 4–7 | Gradual improvement; swelling decreasing | 2–4 |
| Days 7–14 | Minimal discomfort; tenderness when touching area | 1–2 |
| 2+ weeks | Should be mostly pain-free | 0–1 |
Key insight: Pain should follow a downward trend. If your pain is getting worse after day 3, or if it goes away and then comes back, that's a red flag that needs professional attention.
Best Pain Medications After Implant Surgery
Research published in the Journal of Oral and Maxillofacial Surgery shows that the combination of ibuprofen + acetaminophen is as effective as opioids for post-dental surgery pain, without the addiction risk or side effects.
The Alternating Method (Most Effective)
This is what implant surgeons increasingly recommend:
- Hour 0: Take 600mg ibuprofen (3 × 200mg tablets) with food
- Hour 3: Take 500mg acetaminophen (1 extra-strength Tylenol)
- Hour 6: Take 600mg ibuprofen again
- Hour 9: Take 500mg acetaminophen again
- Continue alternating for the first 48–72 hours
This approach provides continuous pain relief because as one medication starts wearing off, the other kicks in. The two drugs work through different mechanisms — ibuprofen reduces inflammation at the source, while acetaminophen blocks pain signals in the brain.
Medications to Avoid
- Aspirin: Thins blood and can increase bleeding at the surgical site
- Blood thinners: Only stop if your doctor explicitly tells you to
- Opioids: Only if prescribed by your surgeon for severe bone grafting cases. Not first-line treatment
Pro tip: Start your pain medication before the anesthesia wears off. If you wait until you're already in pain, you're playing catch-up. Your surgeon should tell you when to take your first dose — typically right after the procedure.
Ice Therapy: The 48-Hour Rule
Cold therapy is your best friend for the first 48 hours. Here's how to do it correctly:
- Apply an ice pack (or a bag of frozen peas wrapped in a thin towel) to the outside of your cheek over the implant area
- Follow the 20 minutes on, 20 minutes off cycle
- Continue this pattern as much as possible during waking hours for the first 48 hours
- After 48 hours, switch to warm compresses — heat increases blood flow and helps with remaining swelling
Never apply ice directly to skin — always use a cloth barrier. And never apply ice to the inside of your mouth near the surgical site.
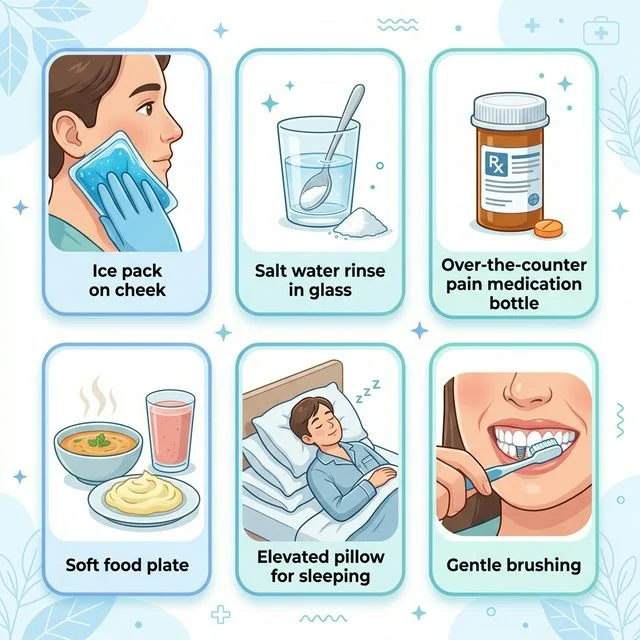
Salt Water Rinses
Salt water is a gentle antimicrobial that reduces bacteria, soothes inflamed tissue, and promotes healing. But timing matters:
- First 24 hours: Do NOT rinse at all. The blood clot forming at the surgical site is critical for healing. Rinsing can dislodge it
- After 24 hours: Mix ½ teaspoon of salt in 8 oz of warm water
- Gently swish (don't gargle vigorously) for 30 seconds, then let it fall out of your mouth rather than spitting forcefully
- Rinse 4–6 times daily, especially after meals, for the first 1–2 weeks
Some dentists recommend adding a small amount of baking soda to the salt water for extra antimicrobial effect. Ask your surgeon if this is appropriate for your case.
Diet Modifications for Pain Relief
What you eat in the first two weeks directly affects your pain level. Chewing on or near the implant site causes trauma to healing tissue.
Days 1–3: Liquids and Very Soft Foods Only
- Smoothies (no straws — suction can dislodge the blood clot)
- Bone broth and warm (not hot) soups
- Yogurt, pudding, applesauce
- Mashed potatoes, scrambled eggs
- Protein shakes for nutrition
Days 4–14: Soft Foods
- Pasta, soft-cooked rice
- Steamed vegetables (well-cooked and soft)
- Fish, soft bread
- Avocado, bananas
Foods to Avoid for 2+ Weeks
- Anything crunchy: chips, nuts, raw carrots, popcorn
- Chewy or sticky foods: caramel, gummy candy, tough steak
- Spicy foods: irritate the surgical site
- Very hot foods: can increase bleeding and inflammation
- Alcohol: interferes with healing and interacts with pain medications
How to Sleep After Implant Surgery
The right sleeping position significantly reduces swelling and pain:
- Elevate your head at a 30–45° angle using 2–3 pillows. This reduces blood flow to the head and minimizes swelling. Sleep in a recliner if you have one
- Sleep on the opposite side from the implant. Pressure on the surgical side increases pain and swelling
- Take your evening pain medication 30 minutes before bed so it kicks in as you fall asleep
- Place a towel on your pillow — minor blood-tinged drooling is normal the first night
Most patients find the first two nights are the hardest for sleep. By night 3–4, sleeping becomes much easier as swelling decreases.
Natural Pain Relief Methods
These methods can supplement (not replace) your medication routine:
Clove Oil (Eugenol)
Clove oil has been used in dentistry for centuries as a natural anesthetic. It contains eugenol, which has both analgesic and antibacterial properties. Dab a tiny amount on a cotton ball and gently apply near (not on) the surgical site. However, ask your dentist first — some surgeons don't recommend it near fresh implant sites.
Chamomile Tea
Chamomile has anti-inflammatory properties. After the first 24 hours, brew a cup of chamomile tea, let it cool to lukewarm, and use it as a gentle mouth rinse. You can also apply a cooled chamomile tea bag to the site.
Turmeric Paste
Curcumin (the active compound in turmeric) is a potent anti-inflammatory. Some patients find relief by mixing turmeric powder with a small amount of water and gently dabbing it near the area. Research supports turmeric's role in natural inflammation management for oral health.
Deep Breathing and Relaxation
Stress and tension increase pain perception. Practicing deep breathing (inhale for 4 counts, hold for 4, exhale for 4) activates your parasympathetic nervous system and can reduce your experience of pain by up to 30%.
When Pain Signals a Problem
Call your dentist immediately if you experience any of the following:
- Pain that intensifies after day 3–4 instead of improving
- Pain that returns after a period of improvement (day 7+)
- Throbbing pain that doesn't respond to ibuprofen + acetaminophen
- Fever over 101°F (38.3°C)
- Swelling that gets worse after 72 hours or spreads
- Pus or foul-tasting discharge from the implant site
- The implant feels loose or moves when you touch it
- Numbness or tingling in your lip, chin, or tongue that doesn't resolve (possible nerve damage)
- Difficulty opening your mouth wider than 2 fingers after a week
These symptoms may indicate infection, implant failure, or nerve damage — all of which require prompt treatment. Early intervention dramatically improves outcomes.
Managing Pain Weeks or Months Later
If you're experiencing pain long after the initial healing period, the causes are different from immediate post-surgical pain:
Peri-Implantitis
An infection of the tissue and bone around the implant that causes pain, swelling, and bleeding. It's the implant equivalent of gum disease. Treatment involves professional cleaning and sometimes antibiotics. If caught early, the implant can usually be saved. Learn more about proper implant cleaning to prevent this.
Implant Overloading
If you started chewing hard foods too soon or if your bite isn't properly aligned, excessive force on the implant can cause persistent pain. Your dentist can check your bite with articulating paper and make adjustments.
Nerve Damage
A rare complication that causes pain, tingling, or numbness in the lower lip, chin, or tongue. This usually happens with lower jaw implants placed too close to the inferior alveolar nerve. Most cases resolve on their own within 3–6 months, but some require specialist intervention.
Sinus Issues (Upper Implants)
Upper jaw implants that protrude into the sinus cavity can cause chronic sinus pain or recurring sinus-related dental pain. This may require surgical revision.
Implant Rejection
Extremely rare, but the body can fail to integrate with the titanium post. Signs include persistent pain, mobility, and bone loss visible on X-ray. The implant needs to be removed, the area healed, and a new attempt made.
Frequently Asked Questions
Learn more about dental implants:
Read Our Complete Dental Implants Guide →