Here's something most people don't realize: gum disease is the #1 cause of tooth loss in adults — not cavities. You can have zero cavities and still lose teeth because infected gums destroy the bone holding your teeth in place. And by the time you notice symptoms, significant damage may already be done.
The scariest part? Gum disease is usually painless in its early stages. No toothache to warn you, no sensitivity to trigger an emergency visit. Just slowly progressing infection that silently eats away at your gum tissue and jawbone.
What Healthy Gums Look Like
Before you can identify problems, know what normal looks like:
- Color: Pink (or dark pink/brown in darker-skinned individuals — totally normal)
- Texture: Firm, stippled (like orange peel texture)
- Bleeding: None. Healthy gums don't bleed when you brush or floss.
- Shape: Pointed triangles between teeth (papillae), scalloped around each tooth
- Smell: No persistent bad breath (halitosis)
Gum Disease: Gingivitis vs. Periodontitis
| Feature | Gingivitis | Periodontitis |
|---|---|---|
| Severity | Mild (inflammation only) | Serious (bone loss) |
| Reversible? | ✅ Yes, completely | ❌ Bone loss is permanent |
| Bleeding | When brushing/flossing | Often spontaneous |
| Gum pockets | 1–3mm (normal) | 4mm+ (problematic) |
| Bone loss | None | Progressive |
| Tooth looseness | None | Advanced stages |
| Treatment | Better hygiene + cleaning | Deep cleaning, surgery, ongoing maintenance |
Gingivitis: the reversible stage
Plaque builds up at the gumline, bacteria irritate the tissue, gums become red, puffy, and bleed easily. The good news: gingivitis is 100% reversible with improved brushing, daily flossing, and a professional cleaning. It typically resolves within 2–4 weeks of consistent care. No permanent damage is done.
Periodontitis: the destructive stage
When gingivitis is ignored, bacteria migrate below the gumline and start destroying the bone and connective tissue that holds teeth in place. This creates "pockets" — deep spaces between the tooth and gum where bacteria thrive beyond your toothbrush's reach. Once bone is lost, it doesn't grow back on its own. This is why early intervention is critical.
Signs of periodontitis: persistent bad breath, loose teeth, receding gums, pus between teeth and gums, changes in bite, teeth that appear longer. If you're noticing loose teeth, read our article on how to tighten a loose tooth for immediate steps.
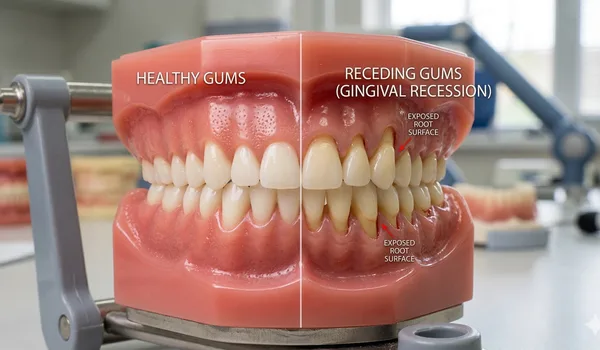
Receding Gums
Gum recession is when gum tissue pulls back from the tooth, exposing the root surface. It's incredibly common — about 50% of adults have some degree of recession. Full details in our complete guide to receding gums.
What causes recession
- Aggressive brushing: The #1 cause in young adults. Using a hard-bristle brush or scrubbing horizontally wears away gum tissue.
- Gum disease: The leading cause in older adults. Bacterial infection destroys gum attachment.
- Genetics: Some people have thinner gum tissue that's more prone to recession.
- Grinding (bruxism): Excessive force on teeth stresses the gum attachment.
- Tobacco use: Reduces blood flow to gums, making them more vulnerable.
- Piercings: Lip and tongue piercings rubbing against gums cause localized recession.
- Orthodontic treatment: Moving teeth outside the bone can cause recession — your orthodontist monitors for this during braces treatment.
Can receding gums grow back?
No. Once gum tissue is lost, it does not regenerate naturally. You can stop further recession through improved technique and treating the underlying cause, but lost tissue requires a gum graft to restore. Some natural approaches can help slow or prevent further recession — we cover them all in our natural remedies for receding gums article.
Deep Cleaning (Scaling & Root Planing)
When regular cleaning isn't enough, your dentist recommends scaling and root planing (SRP) — commonly called a "deep cleaning." This is the primary non-surgical treatment for periodontitis.
What happens during a deep cleaning
- Numbing: Local anesthesia for comfort (not always needed for mild cases)
- Scaling: Ultrasonic and hand instruments remove plaque, tartar, and bacterial toxins from below the gumline — inside the pockets
- Root planing: The root surfaces are smoothed to prevent bacterial reattachment and help gums heal against the tooth
Deep cleaning details
| Detail | Info |
|---|---|
| Duration | 45–60 min per quadrant (typically 2 visits) |
| Cost | $200–$400 per quadrant ($800–$1,600 full mouth) |
| Insurance | Usually covered at 50–80% |
| Recovery | Sore gums for 3–5 days, mild bleeding |
| Follow-up | Re-evaluation in 4–6 weeks + maintenance cleanings every 3–4 months |
After SRP, pockets should shrink as gums heal and reattach to teeth. If pockets remain deep (5mm+) despite good home care, surgical options like flap surgery or bone grafting may be recommended.
Gum Graft Surgery
For significant recession, a gum graft is the gold standard treatment. Tissue is taken from the palate (roof of mouth) or from a donor source and grafted over the exposed root. Full pricing breakdown in our gum graft cost guide.
| Graft Type | Cost Per Tooth | Best For |
|---|---|---|
| Connective tissue graft | $600–$1,200 | Most common; covers exposed roots |
| Free gingival graft | $500–$1,000 | Adding tissue thickness |
| Pedicle graft | $600–$1,200 | When adjacent tissue is adequate |
| AlloDerm (donor tissue) | $700–$1,500 | Avoiding second surgical site |
| Pinhole technique | $800–$2,000 | Multiple teeth, minimally invasive |
Prevention: How to Keep Gums Healthy
- Brush gently with a soft brush: 45-degree angle toward the gumline, gentle circular motions. Electric toothbrushes with pressure sensors are excellent for preventing over-brushing.
- Floss or water floss daily: Gets bacteria from between teeth and below the gumline where brushes can't reach. Same tool used to clean implants.
- Don't smoke: Smoking is the single biggest modifiable risk factor for gum disease. Smokers are 3–6x more likely to develop periodontitis.
- Regular cleanings: Every 6 months for healthy gums, every 3–4 months if you have a history of gum disease. A cleaning takes 20–30 minutes.
- Manage health conditions: Diabetes, autoimmune diseases, and certain medications (blood pressure, anti-seizure) affect gum health.
- Eat well: Vitamin C deficiency directly affects gum tissue. Leafy greens, citrus, and berries support gum health.
Gum Disease and Your Overall Health
Research increasingly links gum disease to serious systemic conditions:
- Heart disease: People with periodontitis have a 2–3x higher risk of heart attack and stroke. Bacterial inflammation enters the bloodstream.
- Diabetes: The relationship is bidirectional — diabetes increases gum disease risk, and gum disease makes blood sugar harder to control.
- Pregnancy complications: Periodontitis is associated with preterm birth and low birth weight.
- Alzheimer's disease: P. gingivalis bacteria (the primary periodontal pathogen) has been found in Alzheimer's brain tissue.
- Respiratory disease: Bacteria from infected gums can be aspirated into the lungs.
Taking care of your gums isn't just about keeping your teeth — it's about protecting your entire body.
Frequently Asked Questions
Can receding gums grow back?
Once gum tissue has receded, it cannot grow back on its own. However, early-stage recession can be halted with improved oral hygiene, and advanced recession can be treated with gum grafting surgery, which covers exposed roots with tissue from the palate or a donor source.
What does a gum graft cost?
Gum graft surgery costs $600–$1,200 per tooth or $2,000–$10,000 for multiple teeth. Connective tissue grafts are the most common and cost $700–$1,000 per tooth. Insurance may cover gum grafts when deemed medically necessary for periodontal health.
How do you know if you have gum disease?
Early signs include red or swollen gums, bleeding when brushing or flossing, persistent bad breath, and gum tenderness. Advanced signs include receding gums, loose teeth, pus between teeth, and changes in bite alignment. A dental exam with probing measurements confirms the diagnosis.
Is gum disease reversible?
Gingivitis (early gum disease) is fully reversible with professional cleaning and improved home care. Periodontitis (advanced gum disease) is not reversible but can be managed and controlled with deep cleaning, medication, and possibly surgery to prevent further bone and tissue loss.
Explore Our Gum Health Articles
Related topics
- Tooth Extraction Guide — When gum disease causes tooth loss
- Dental Implants Guide — Replacing teeth lost to periodontal disease
- Fillings Guide — Cavities and gum disease often occur together
- Tooth Pain Guide — When gum problems cause pain
- Braces Guide — Gum health during orthodontic treatment
- General Dental Guide — Routine care to prevent gum disease